
The Man Who Discovered Hand Hygiene But Died Ignored
Ignaz Semmelweis (1818–1865)
2026 World Book Day, a true story from the frontlines of science, sanitation, and human stubbornness.
Table of Contents
ToggleA Hospital That Killed More Than It Cured
Vienna, 1847. The Habsburg Empire is at its height. The city is a centre of culture, medicine, and intellectual ambition. And inside the Vienna general hospital, women are dying.
Not from war. Not from famine. From giving birth.
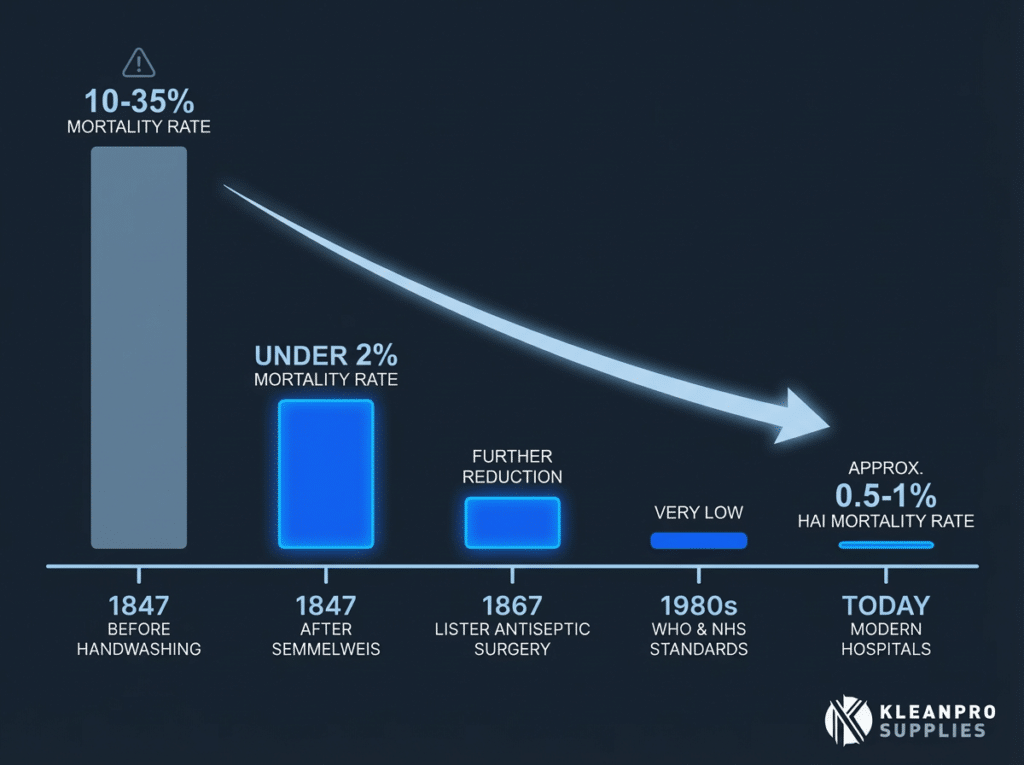
The first obstetrical clinic at the Vienna general hospital had a mortality rate from childbed fever, known medically as puerperal fever, that hovered between 10% and 35% in its worst months. In some periods, one in three women who gave birth there did not survive. Women begged to deliver in the streets rather than be admitted. Some faked labour to avoid the ward. The fear was rational. The death toll was real. And nobody, not a single doctor in that prestigious institution, could explain why.
What made it worse was that the second obstetrical clinic, just down the corridor, had a mortality rate of roughly 2%. Same hospital, same city. Wildly different outcomes. The difference? One clinic was staffed by medical students and doctors. The other was staffed by midwives.
This was the world that Ignaz Semmelweis walked into. And what he discovered there would change medicine forever, even if it nearly destroyed him first.

The Man Behind the Discovery
Ignaz Philipp Semmelweis was born in Buda, Hungary, in 1818, the fifth child of a prosperous grocer. He studied law briefly before switching to medicine, completing his degree in Vienna in 1844. By 1846, he had secured a position as an assistant in the first obstetrical clinic under Professor Johann Klein, one of the most respected obstetricians in Europe.
Semmelweis was, by all accounts, a meticulous observer. He was not a theorist by nature. He was a man who watched, measured, and questioned. And from the moment he arrived at the clinic, the disparity in death rates between the two wards consumed him.
He was not the first to notice it. But he was the first to do something systematic about it.
He began eliminating variables. Could it be the position of delivery? The overcrowding? The diet of the patients? The ventilation? One by one, he ruled them out. The answer came not from a laboratory, but from a tragedy.
In early 1847, a close friend and colleague, Jakob Kolletschka, died after being accidentally cut with a scalpel during a post-mortem examination. The pathology report on Kolletschka’s death described lesions and tissue changes almost identical to those found in women who had died of childbed fever.
Semmelweis made the connection immediately. The doctors and medical students in the first clinic were moving directly from performing autopsies to delivering babies, often without washing their hands at all. The midwives in the second clinic did not perform autopsies. They had no contact with cadavers.
He called it “cadaverous particles.” We would call it bacterial contamination. The terminology was different. The insight was the same.
The Discovery – Data, Chlorine, and a Simple Protocol
In May 1847, Semmelweis introduced a mandatory handwashing protocol using chlorinated lime solution, what we would recognise today as a precursor to modern antiseptic hand hygiene. He required all medical staff to wash their hands before entering the maternity ward and before examining patients.
The results were immediate and dramatic.
Within months, the mortality rate in the first clinic dropped from over 10% to below 2%, bringing it in line with the midwife led second clinic. In some months, the death rate fell to less than 1%.
“It is the duty of all of us to acknowledge our errors and to correct them.” — Said Ignaz Semmelweis, The Etiology, Concept, and Prophylaxis of Childbed Fever, 1861
He had not just observed a pattern. He had intervened, measured the outcome, and proven causation through consistent, repeatable results. By any modern standard of evidence based medicine, this was a landmark finding.
The Resistance – When Truth Is Too Inconvenient
Here is where the story takes a darker turn.
You might expect that a discovery this clear, this well evidenced, this immediately life saving, would be celebrated. You would be wrong.
The medical establishment of mid-19th century Europe was not ready for what Semmelweis was suggesting. Germ theory had not yet been established. Louis Pasteur would not publish his foundational work until the 1860s. Joseph Lister would not introduce antiseptic surgical technique until 1867. In 1847, the dominant belief was that disease arose from “miasma,” bad air, or internal imbalances. The idea that doctors themselves were the vectors of death was not just scientifically unaccepted, it was socially intolerable.
To accept Semmelweis’s findings was to accept that physicians, educated men of standing, had been killing their patients with unwashed hands. The professional and psychological cost of that admission was enormous. And so, rather than accept the evidence, many chose to reject the messenger.
Professor Klein, Semmelweis’s own superior, was openly hostile. Prominent physicians across Europe dismissed his findings. Some argued his data was flawed. Others suggested the improvement in mortality was coincidental. A few simply refused to engage with the evidence at all.
Semmelweis, for his part, was not a diplomat. He was passionate, increasingly frustrated, and at times confrontational. He wrote open letters accusing his critics of being responsible for the deaths of thousands of women. He called out colleagues by name. His manner alienated potential allies. The scientific community, already resistant, closed ranks further.
He was not renewed in his position in Vienna. He returned to Budapest, where he continued his work and achieved similar results at the St. Rochus Hospital. But the international recognition he deserved never came. His major work, “The Etiology, Concept, And Prophylaxis Of Childbed Fever”, published in 1861, was largely ignored or poorly reviewed.

The Tragedy – A Death That Proved His Point
By 1865, Semmelweis was in serious mental decline. The years of rejection, the weight of knowing that women continued to die unnecessarily, and what may have been early onset dementia or another neurological condition had taken their toll. In July of that year, colleagues arranged for him to be committed to a mental asylum in Vienna.
He died there on 13 August 1865, just two weeks after his admission. He was 47 years old.
The official cause of death was septicaemia, a systemic blood infection. Some historians believe it may have been caused by a wound sustained during a beating by asylum guards. Others suggest he contracted an infection during a surgical procedure shortly before his death.
The cruel irony is almost unbearable. The man who had spent nearly two decades trying to prevent the spread of infection through contaminated contact may have died from exactly that. A wound. An unclean environment. The very mechanism of death he had identified and fought against, turned against him in his final days.
He died without recognition. He died without vindication. He died, in many ways, as he had lived in his final years, alone, dismissed, and ahead of his time.
The Vindication – Science Catches Up
History, at least, corrected itself.
In the 1860s, Louis Pasteur’s germ theory of disease established the scientific framework that explained everything Semmelweis had observed. Microorganisms, not miasma, caused infection. Contamination was real, measurable, and preventable.
Joseph Lister, building directly on Pasteur’s work, introduced antiseptic technique into surgery in 1867, using carbolic acid to sterilise instruments and wounds. The results mirrored what Semmelweis had achieved two decades earlier. Infection rates fell. Patients survived. The medical world, this time, listened.
Semmelweis was gradually rehabilitated in the historical record. Statues were erected. Streets were named after him. His portrait appeared on Hungarian currency. The term “Semmelweis reflex” entered the lexicon, describing the instinctive rejection of new information that contradicts established norms, a phenomenon his story had illustrated with devastating clarity.
The world health organization(WHO), the NHS, the centers for disease control and prevention(CDC), and the European centre for disease prevention and control(ECDC) all now recognise hand hygiene as one of the single most effective interventions in infection prevention. Every protocol, every guideline, every hand hygiene campaign in every hospital in the world traces its lineage, directly or indirectly, back to a Hungarian physician in a Vienna maternity ward in 1847.

Why It Still Matters – From Vienna to Your Workplace
The story of Semmelweis is not just history. It is a live issue.
Healthcare associated infections, known as HAIs, remain one of the most significant challenges facing health systems globally. According to the UK Health Security Agency, approximately 300,000 patients in England acquire a healthcare associated infection each year, contributing to thousands of preventable deaths and costing the NHS an estimated £2.7 billion annually.
“If every healthcare worker cleaned their hands at the right times, we could prevent millions of infections and save hundreds of thousands of lives every year.” — World Health Organization, Clean Care Is Safer Care Programme
The WHO’s “5 Moments for Hand Hygiene” framework, now adopted by health systems worldwide including the NHS, identifies the five critical points at which hand hygiene must occur in clinical settings: before touching a patient, before a clean or aseptic procedure, after body fluid exposure, after touching a patient, and after touching patient surroundings.
These are not bureaucratic checkboxes. They are the direct descendants of Semmelweis’s original observation, that the hands of caregivers can carry contamination from one surface to another, and that breaking that chain saves lives.
But the lesson extends far beyond hospitals. In commercial kitchens, food preparation areas, office environments, schools, care homes, and public facing businesses, the same principle applies. Contamination travels on surfaces. It travels on hands. It travels through the products we use to clean, or fail to clean, those surfaces properly.
The NHS provides clear guidance on correct handwashing technique, including the use of soap and water for a minimum of 20 seconds, covering all surfaces of the hand including between fingers and under nails. This guidance is grounded in the same evidence base that Semmelweis began building in 1847.
“In England, around 300,000 patients a year acquire a healthcare associated infection as a direct result of care.” — Quote by the UK Health Security Agency, in 2023.
Proper hand hygiene is not just a clinical matter. It is a professional standard. And the products used to support it, whether in a hospital ward, a restaurant kitchen, or a care facility, must be fit for purpose.
The KleanPro Connection
Standards That Semmelweis Would Recognise
Semmelweis did not have access to modern chemistry. He worked with chlorinated lime because it was the best available tool. What he understood, with absolute clarity, was that the quality and consistency of the hygiene intervention mattered. A half hearted wash with an ineffective solution was not enough. The protocol had to be right. The product had to work.
That principle has not changed.
At KleanPro Supplies, we supply professional grade cleaning and hygiene products to commercial and residential customers across the UK. As the exclusive UK distributor of Mistolin Pro, a brand with over 50 years of European manufacturing expertise, we are committed to providing products that meet the highest standards of performance and safety.
Mistolin Pro products are manufactured to ISO 9001 (quality management), ISO 14001 (environmental management), and ISO 45001 (occupational health and safety) standards. These are not marketing claims. They are independently verified certifications that reflect a genuine commitment to consistent, effective, and responsible formulation.
Whether you are managing a commercial kitchen, running a care facility, or simply maintaining a clean and safe environment at home, the products you use matter. Semmelweis understood that. We do too.
Reading Suggestions
“The Doctors’ Plague – Germs, Childbed Fever, And The Strange Story Of Ignac Semmelweis” by Sherwin B. Nuland
If this story has stayed with you, and we hope it has, Nuland’s biography is the place to go next. Written with the precision of a surgeon and the empathy of a storyteller, it traces Semmelweis’s life from his early promise in Budapest to his tragic end in Vienna, never losing sight of the human being behind the discovery. It is a book about science, yes, but more than that, it is a book about what happens when the truth is too uncomfortable for the world to accept. Read it slowly. It deserves that.
Published By KleanPro Supplies On World Book Day 2026

